GET YOUR LIFESTYLE BACK!
Providing Superior Health Through Integrative Medicine
Producing Outstanding Results For Our Patients
Stop Suffering Needlessly
Welcome To Neck Back and Knee Center. Responsible Pain Management in Florence, Kentucky. We are dedicated to staying on top of the latest tools and treatments. It is our goal to create a friendly and professional atmosphere that you can rely on for all of your needs.
We couldn’t be the office we are without our staff. They are always helping patients by giving them the information they need to make the right decision. Our staff will discuss all of your options and what to expect. They are here to answer your questions and address your concerns. It is their goal to give you a satisfying experience every time you walk through our doors. Quite simply, they are great at what they do!
We welcome new patients and strive to give our patients the very best care available. We also work hard to make sure to offer the most up-to-date services so that you are able to walk out of each appointment feeling even better than you did after the last one. It is always our goal to improve your life.
When visiting us, you should expect nothing but the absolute best. That is our goal. We appreciate your business and truly look forward to serving you in the future. If you have any questions regarding our services or your first visit, contact us today at 859-283-2475.
Same Day Pain Relief
Shoulder and Neck Pain
We offer one of the newest and most cutting-edge therapies for chronic shoulder and neck pain.
Back Pain
This therapy has significant potential for those in pain, and could actually repair structural problems while treating pain and inflammation simultaneously.
Wrist, Hand & Elbow Pain
Cellular therapy is one of the most innovative approaches to chronic joint pain.
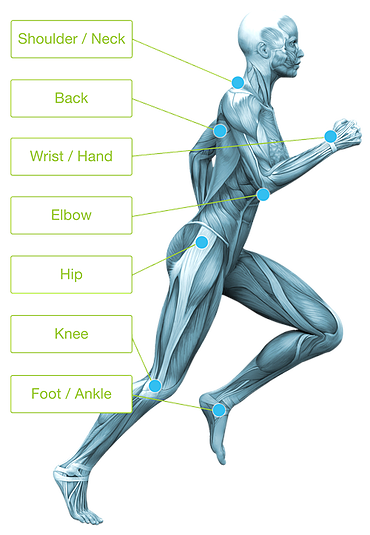
Hip Pain
When running and walking become painful, Cellular therapy can be the option for relief.
Knee Pain
This therapy has the potential to actually alter the course of the condition and not simply mask the pain.
Foot and Ankle Pain
This therapy stimulates the body to repair the foot ligaments. It does so by inducing a mild inflammatory reaction in the weakened ligaments and cartilage.
Currently Treating The Following Areas

RESTORATIVE MEDICINE
CLICK HERE TO LEARN MORE

Auto Injuries
CLICK HERE TO LEARN MORE

Spinal decompression
CLICK HERE TO LEARN MORE
Stop Suffering Needlessly
Our Services

Sports Injury
CLICK HERE TO LEARN MORE
Back Pain
CLICK HERE TO LEARN MORE

Neck Pain
CLICK HERE TO LEARN MORE
Shoulder Pain
CLICK HERE TO LEARN MORE

Auto Injuries
CLICK HERE TO LEARN MORE
HIP PAIN
CLICK HERE TO LEARN MORE

Headaches/Migraines
CLICK HERE TO LEARN MORE
Knee Pain
CLICK HERE TO LEARN MORE
Neuropathy
CLICK HERE TO LEARN MORE
Sciatica
CLICK HERE TO LEARN MORE
Pinched Nerve
CLICK HERE TO LEARN MORE

Whiplash
CLICK HERE TO LEARN MORE
Bulging Herniated Disc
CLICK HERE TO LEARN MORE
IV Therapy
CLICK HERE TO LEARN MORE
Arthritis
CLICK HERE TO LEARN MORE

CareCredit® is an easy way to pay for healthcare expenses and daily medical needs
based on your credit worthiness. Get approved in minutes for CareCredit®
Use your virtual card immediately to cover your visit today.
Patient Testimonials


























These Are Just A Few of The Many 5-Star Video Testimonials We Have To Share.
We Saved A Space For Your Success Story.
These Are Just A Few of The Many 5-Star Video Testimonials We Have To Share.
We Saved A Space For Your Success Story.
FLORENCE LOCATION
Neck Back and Knee Center
7560 US Hwy 42
Florence, KY 41042
Phone: 859-283-2475
HEBRON LOCATION
Neck Back and Knee Center
2030 Northside Drive
Hebron, KY 41048
Phone: 859-372-0888
CLINIC HOURS
Monday
9:00 am - 1:00 pm
3:00 pm - 6:30 pm
Tuesday
9:00 am - 1:00 pm
3:00 pm - 6:00 pm
Wednesday
9:00 am - 1:00 pm
3:00 pm - 6:00 pm

